release time:2022-07-20 15:54:02
In a conventional hematology meter, red blood cells (RBC) and platelets (PLT) share a single measurement channel. The determination of hemoglobin content (HGB) is the same in any type and grade of hematology analyzer. White blood cell counting and classification has its own dedicated channel. The technical methods and principles used for each test item on the hematology analyzer are briefly described.
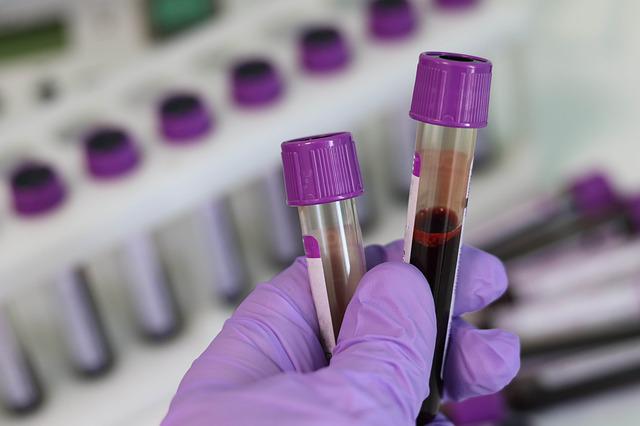
Due to the obvious difference between platelet and red blood cell volumes, it is easy to distinguish the photoelectric signals measured at the same time with a limited threshold. Therefore, to date, a common analysis system has been used for platelet and erythrocyte testing in whole blood analysis. However, there is often a crossover between platelet and red blood cell measurement signals. For example, the pulse signal of a large platelet may be mistaken for a red blood cell and counted. The pulse signal of small red blood cells may enter the platelet channel. This can result in experimental errors. Various manufacturers of hematology analyzers use various advanced technologies to reduce the interference of platelet counts. We describe each of these techniques below:
Sweep Flow
Since platelets and red blood cells are counted in the same counting cell, the cell volume is large, and the platelets can be counted in the same pool. The cells are large in size and form a large pulse when they pass through the central counting induction zone. If there is reflux, a small pulse is formed at the same time due to the eddy current re-entering the edge of the sensing zone, so that the electrode may sense a small pulse equivalent to the size of platelets, resulting in a false increase in platelet count.
The sweep flow technique is to have a steady stream of fluid pass behind the red blood cell counting aperture while the red blood cell and platelet counts are being performed. This allows the red blood cells to be washed away immediately afterwards to prevent them from returning to the sensing area to be counted as platelets.
Hematology Analyzer History
Since the introduction of the Automated Heamatology Analyzer in the 1950s, automated blood cell analysis has evolved from a single electrical impedance technique to a fusion of multiple techniques. These include physics, chemistry, immunology, flow cytometry, information processing techniques, volumetric conduction light scattering (VCS), and multi-angle polarized light scattering (MAPSS). This blood technology has led to more accurate and reliable results for the analysis of various blood cells.
Automated blood cell analysis has evolved from a single semi-automatic unclassified to 3/5-part differential to an automated blood cell analysis pipeline. The processes of complete blood count (CBC), reticulocyte (Ret) count, peripheral blood pushing and staining are fully automated.
Hematology Analyzer Clinical Applications
2023-05-26
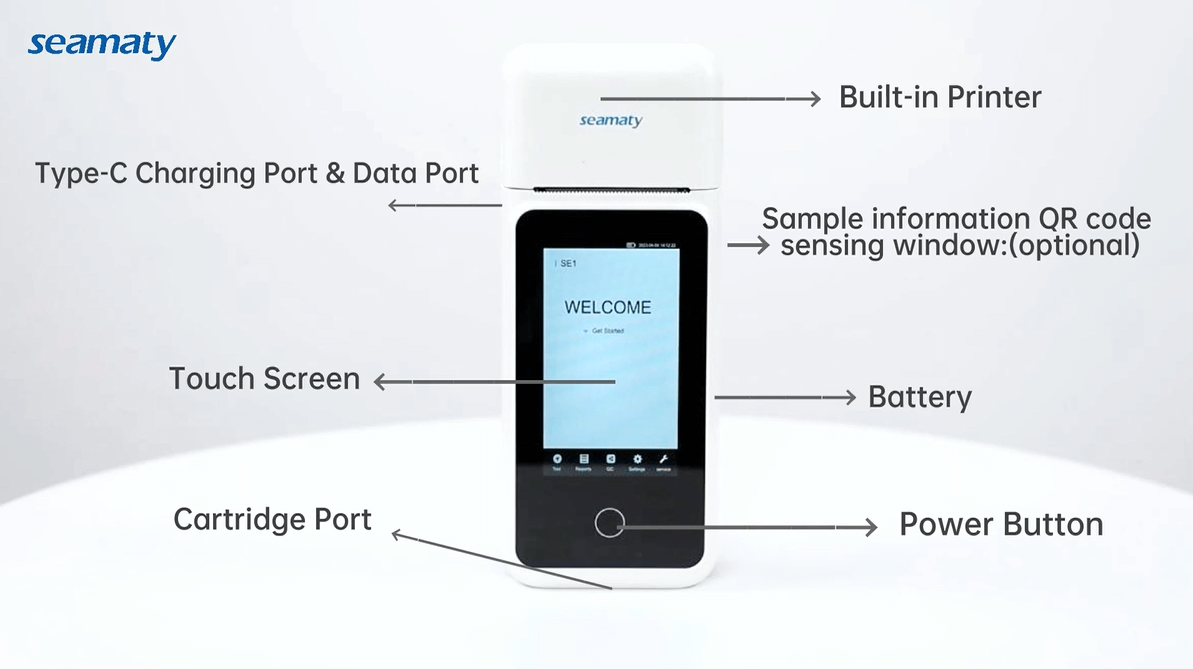
Discover how Seamaty SE1, a handheld electrolyte analyzer, enhances patient care in various healthcare settings. Explore its features, including accurate measurements, versatile sample handling, and maintenance-free operation.
2023-04-25
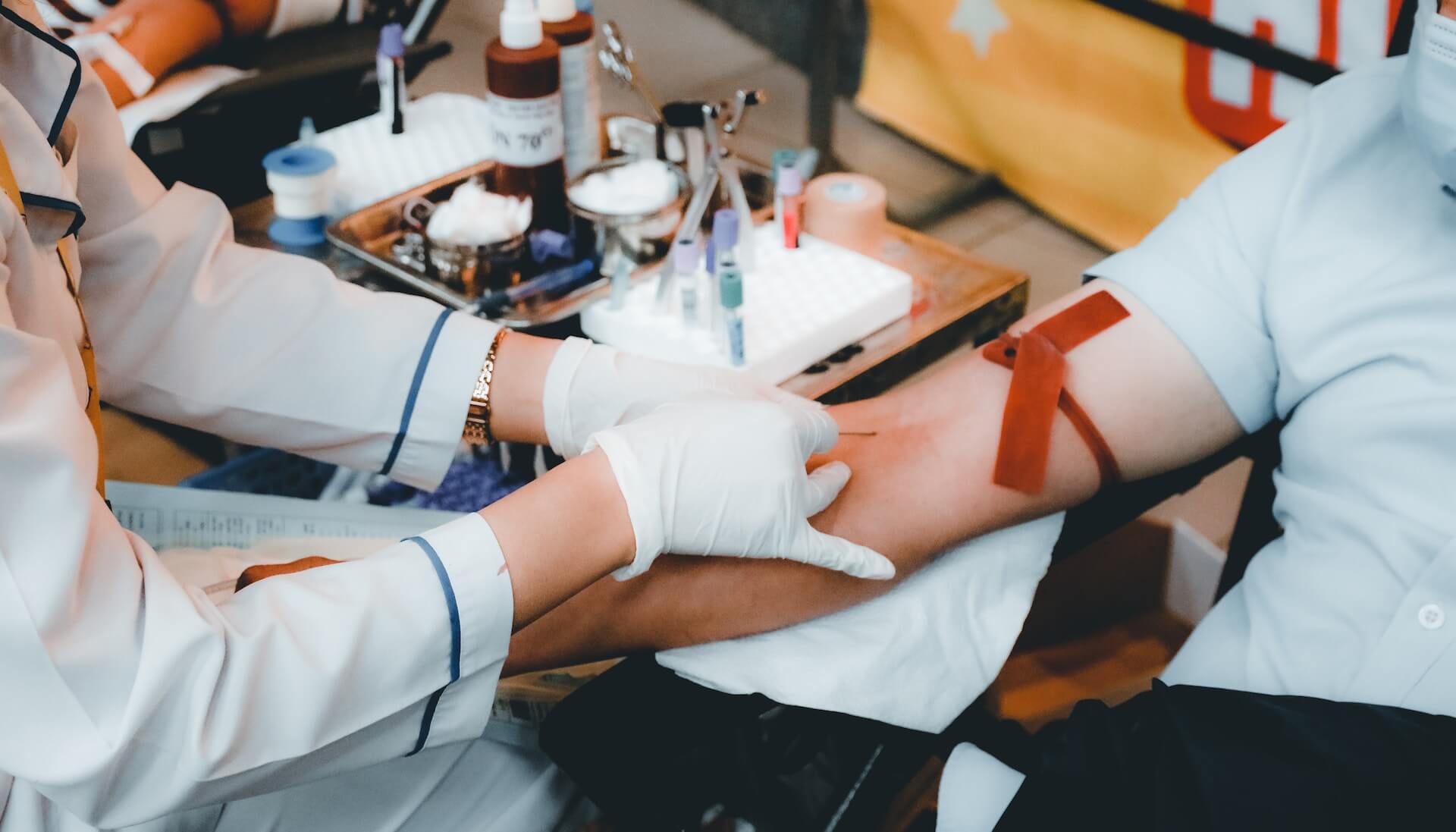
This beginner's guide to blood tests explains what they are, how they work, and what they can detect. Learn about the five main types of blood tests and how to prepare for them.

2022-07-15
This article focuses on molecular diagnostics, a segment of in vitro diagnostics. Molecular diagnostics is the fastest growing in vitro diagnostic field in recent years, and is expected to maintain a high growth rate of 30-50% in the next 3-5 years.